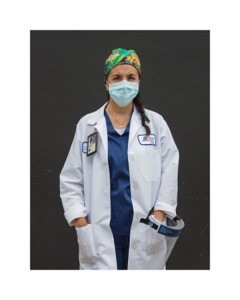
Note: Although Social Worker Lilian Espinoza, LCSW, ACHP-SW, the Assistant Director of the Inpatient Palliative Care Medicine Consultation Service at Mount Sinai Hospital of Queens contracted the novel coronavirus in March and it took her a month to recover, she went right back to work. Here is her story:
By Lilian Espinoza, LCSW, ACHP-SW
Throughout the Covid-19 pandemic, our Palliative Care Service has become one of the most crucial services in the hospital. Located in Queens, a county tremendously impacted by Covid-19, we responded to one of the highest rates of coronavirus infections and deaths in NY. I, too, became part of such statistics as I contracted the virus in early March. While recovery was difficult, with the support of my family and friends, I was able to pull through.
Dedicated to Social Work
I achieved my undergraduate and graduate degrees from Hunter College in New York City. Currently, I am the Assistant Director of the Inpatient Palliative Care Medicine Consultation service at Mount Sinai Hospital of Queens (MSQ). As a Licensed Clinical Social Worker, I have worked with seriously ill and End-of-Life care patients for more than 20 years. In 2004, I became the co-founder of our Palliative Care consultation service at Mount Sinai Hospital of Queens. Since 2004, our Palliative Care mission has been to provide compassionate care, dignity and respect to seriously ill and End-of-Life care patients and their families.
In the early 1980s, during the start of the AIDS Pandemic, I worked with seriously ill patients as one of the first students to be part of the Hunter College HIV/AIDS student internship program. During this time, I quickly learned that an HIV/AIDS diagnosis had a serious impact on a patient’s social and emotional state. Patients were left isolated, stigmatized and under served. Having experienced the AIDS pandemic first-hand, I was motivated to raise awareness, to advocate and support those infected and affected by HIV and AIDS.
Working through all the challenges of the AIDS pandemic has prepared me to do my present work in palliative care during this current Covid-19 Pandemic.
Throughout this pandemic, our Palliative Care Service has become one of the most crucial services in the hospital. Located in Queens, a county tremendously impacted by Covid-19, we responded to one of the highest rates of coronavirus infections and deaths in New York.
During the apex of the epidemic in April, I was finally able to return to work at MSQ, at which point it was apparent that we had transitioned to become a COVID Hospital.
In early April, 99 percent of our patients were COVID-19 positive. Our consults had quadrupled, caseloads multiplied to 20-40 patients daily and most devastating, our death rate averaged to approximately 20 patients per-day. The waves of the COVID tsunami lasted for weeks, as we found ourselves with daily losses and multiple new cases. We lost patients, colleagues, family members, and friends. Our hearts were broken, but we continued to move forward and support those that needed us the most.
 As a Palliative Care team, we assisted to establish patient’s advance directives, goals of care, symptom management, End-of-Life care and more.
As a Palliative Care team, we assisted to establish patient’s advance directives, goals of care, symptom management, End-of-Life care and more.
The uniqueness of this illness, and the subsequent No-Visitor policy, brought about challenges not only for the patients and their families but for our staff as well. The patients and their families experienced isolation, fear, anxiety, great stress and suffering to say the least.
In addition, our Medical teams, staff members where experiencing similar symptoms and also required our support and services.
To support the patients and families and to relieve some of the isolation and suffering, we used iPads and cell phones to visually connect the patient and their families. In my daily work, I became the witness of countless expressions of love, prayers, blessings, tears, kisses and also goodbyes. I had families from all over the world view their loved ones. Some families were stuck in countries such as Colombia and Guatemala and could not return to the U.S. to be with their loved-ones due to travel restrictions. Other families within the states were also unable to travel. Even when the policy changed and one visitor was allowed, many families were simply afraid to come to the hospital for fear of becoming infected.
Whatever their situation was, I know they all had the same common need of connecting one last time with their loved-one.
But for family members, the death of their loved-ones did not end the suffering. The ordeal continued, as family members could not view the bodies, funeral arrangements were delayed. Families could not honor their deceased the way they would have liked nor have proper religious or ritual ceremonies.
A great part of my work has been providing bereavement counseling and assisting the families with funeral arrangements, providing guidance, supporting and resolving complications or delays postmortem. During my postmortem calls, families often expressed gratitude for some closure and the opportunity to have seen their loved-ones, even if they could not touch them.
I feel truly honored and privileged to serve our community as I continue to endure in my work. I continue to use iPads and cell phones, which is a gateway tool for this intimate connection between the patient and family until better days come.
After more than 20 years, practicing my profession as a Social Worker, I know that the many adverse experiences and my continued dedication to Social Work education have molded my vision, which is to continue to do the best work I can do, to serve others, because it really does matter especially during this Covid-19 crisis.
Today more than ever, I embrace my profession and I am proud say: I am Social Worker.
Lilian Espinoza, LCSW, ACHP-SW, the Assistant Director of the Inpatient Palliative Care Medicine Consultation service at Mount Sinai Hospital of Queens (MSQ), says that even though it took her a month to recover, contracting the virus, “gave me more of a reason to come back to support my patients.”
Do you have a front lines story and photos? Please share them with us. Email us at media@socialworkers.org and please be safe.